/ Company
/ Company
/ Company
Zelis
Zelis
Zelis
/ Role
/ Role
/ Role
UX Designer
UX Designer
UX Designer
/ Date
/ Date
/ Date
2023-2024
2023-2024
2023-2024
medical
medical
medical
medical
Price
Price
Price
Price
competition
competition
competition
competition
[1]
[1]
[1]
/ About the project
/ About the project
/ About the project
New legislation required healthcare providers and insurers to publish their rates. We built a product that drives market competition, with the ultimate goal of lowering the cost of care for patients.
New legislation required healthcare providers and insurers to publish their rates. We built a product that drives market competition, with the ultimate goal of lowering the cost of care for patients.
New legislation required healthcare providers and insurers to publish their rates. We built a product that drives market competition, with the ultimate goal of lowering the cost of care for patients.





/ Pricing Leverage
/ Pricing Leverage
/ Pricing Leverage
There's a lack of competitive medical pricing leading to excessive patient expenses, which can be attributed to –
There's a lack of competitive medical pricing leading to excessive patient expenses, which can be attributed to –
There's a lack of competitive medical pricing leading to excessive patient expenses, which can be attributed to –
[01]
[01]
[01]
Opaque pricing structures
Opaque pricing structures
Opaque pricing structures
[02]
[02]
[02]
Complex billing processes
Complex billing processes
Complex billing processes
[03]
[03]
[03]
Market consolidation
Market consolidation
Market consolidation
[04]
[04]
[04]
Negotiation power imbalances
Negotiation power imbalances
Negotiation power imbalances
[05]
[05]
[05]
Limited price transparency
Limited price transparency
Limited price transparency



/ Before
/ Before
/ Before
Insures want more money,
So they increase prices.
Insures want more money,
So they increase prices.
Insures want more money,
So they increase prices.
Patients are financially uninformed,
So they’re forced to pay anything.
Patients are financially uninformed,
So they’re forced to pay anything.
Patients are financially uninformed,
So they’re forced to pay anything.
/ After
/ After
/ After
Users can choose affordable care,
So they steer pricing by demand.
Users can choose affordable care,
So they steer pricing by demand.
Users can choose affordable care,
So they steer pricing by demand.
Insures need to retain members,
So they’re forced to negotiate competitively.
Insures need to retain members,
So they’re forced to negotiate competitively.
Insures need to retain members,
So they’re forced to negotiate competitively.
/ Foundation
/ Foundation
/ Foundation
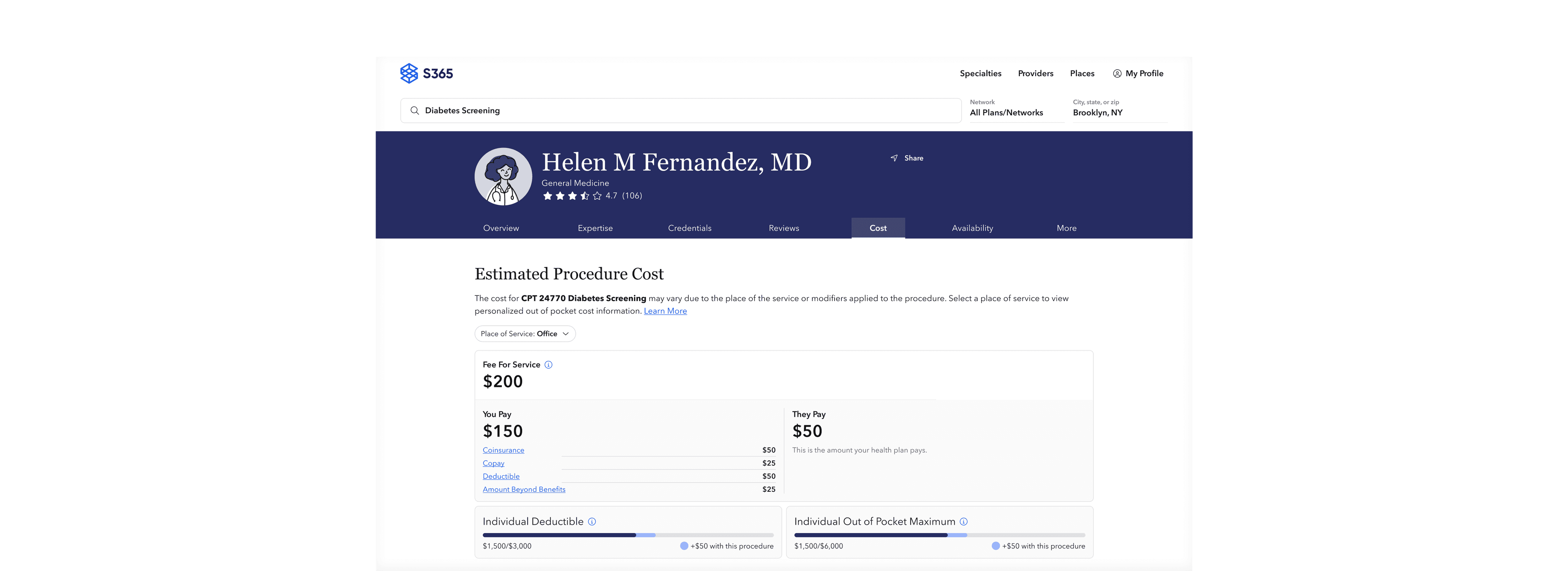
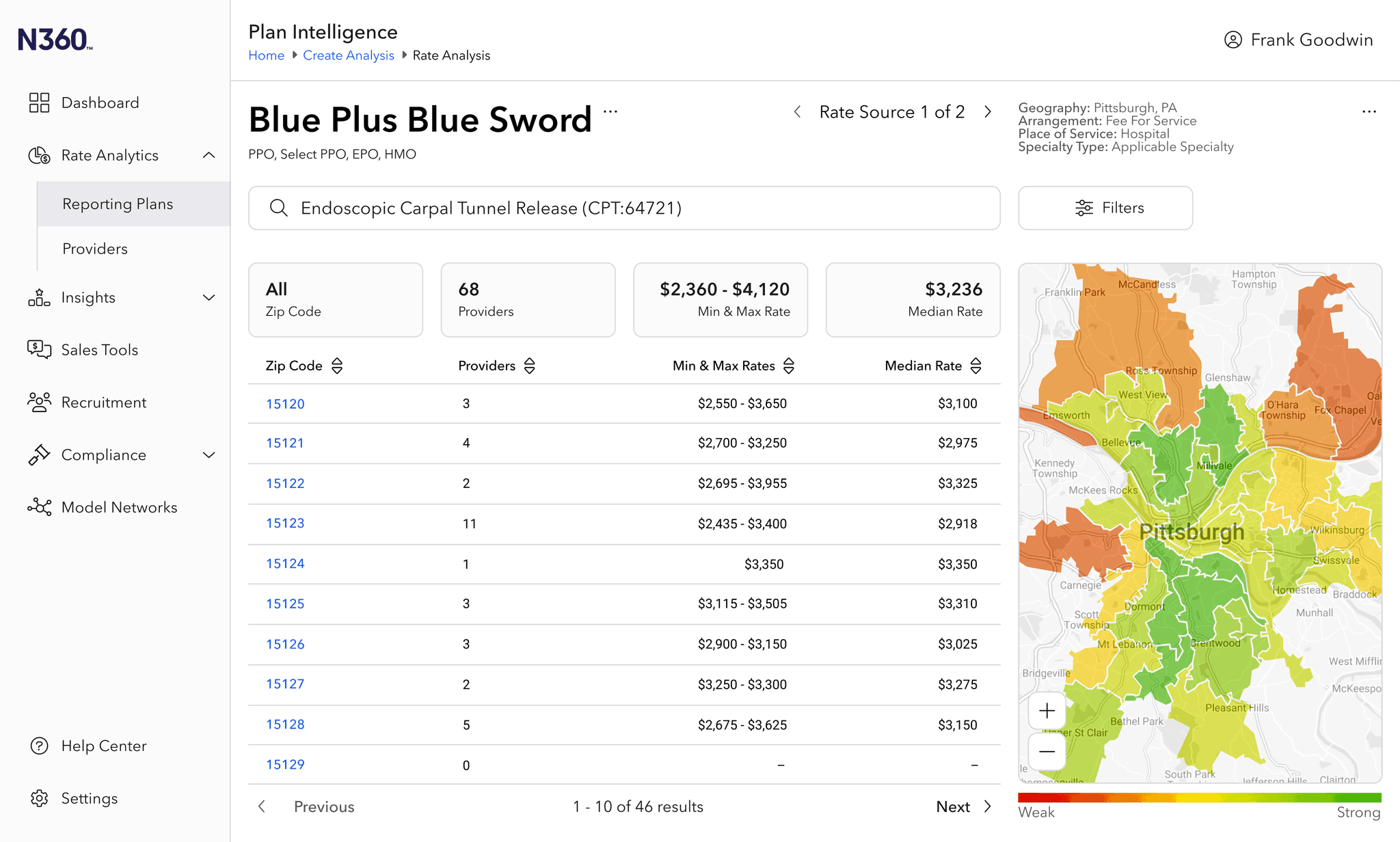
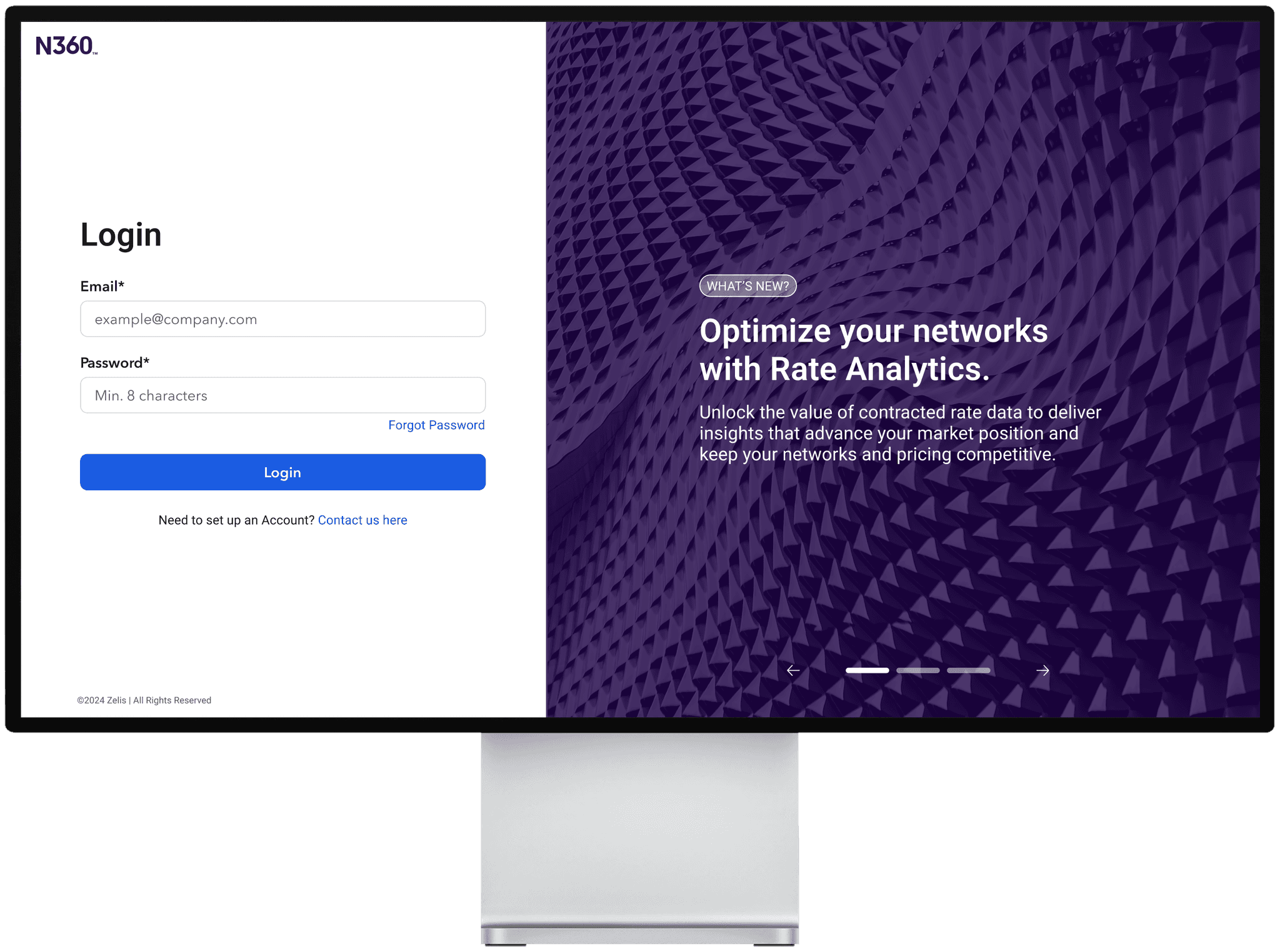
The Network360 tool existed to enable health insurance administrators to see providers in their organizations' networks.
This tool served as the foundation to inject the new pricing data into existing provider profiles and enabled the capability to display competitor pricing insights.
The Network360 tool existed to enable health insurance administrators to see providers in their organizations' networks.
This tool served as the foundation to inject the new pricing data into existing provider profiles and enabled the capability to display competitor pricing insights.
The Network360 tool existed to enable health insurance administrators to see providers in their organizations' networks.
This tool served as the foundation to inject the new pricing data into existing provider profiles and enabled the capability to display competitor pricing insights.


/ Data Isolation
/ Data Isolation
/ Data Isolation

Network
segmentation
Network
segmentation
Network
segmentation

Provider
types
Provider
types
Provider
types

Contracted
services
Contracted
services
Contracted
services

Price distribution
and deviation
Price distribution
and deviation
Price distribution
and deviation

Geographic
network strength
Geographic
network strength
Geographic
network strength

Pricing
Patterns
Pricing
Patterns
Pricing
Patterns


Speaking directly with our clients, we uncovered how users navigate rate negotiations and market insights to inform the granularity of analysis parameters.
Speaking directly with our clients, we uncovered how users navigate rate negotiations and market insights to inform the granularity of analysis parameters.
Speaking directly with our clients, we uncovered how users navigate rate negotiations and market insights to inform the granularity of analysis parameters.
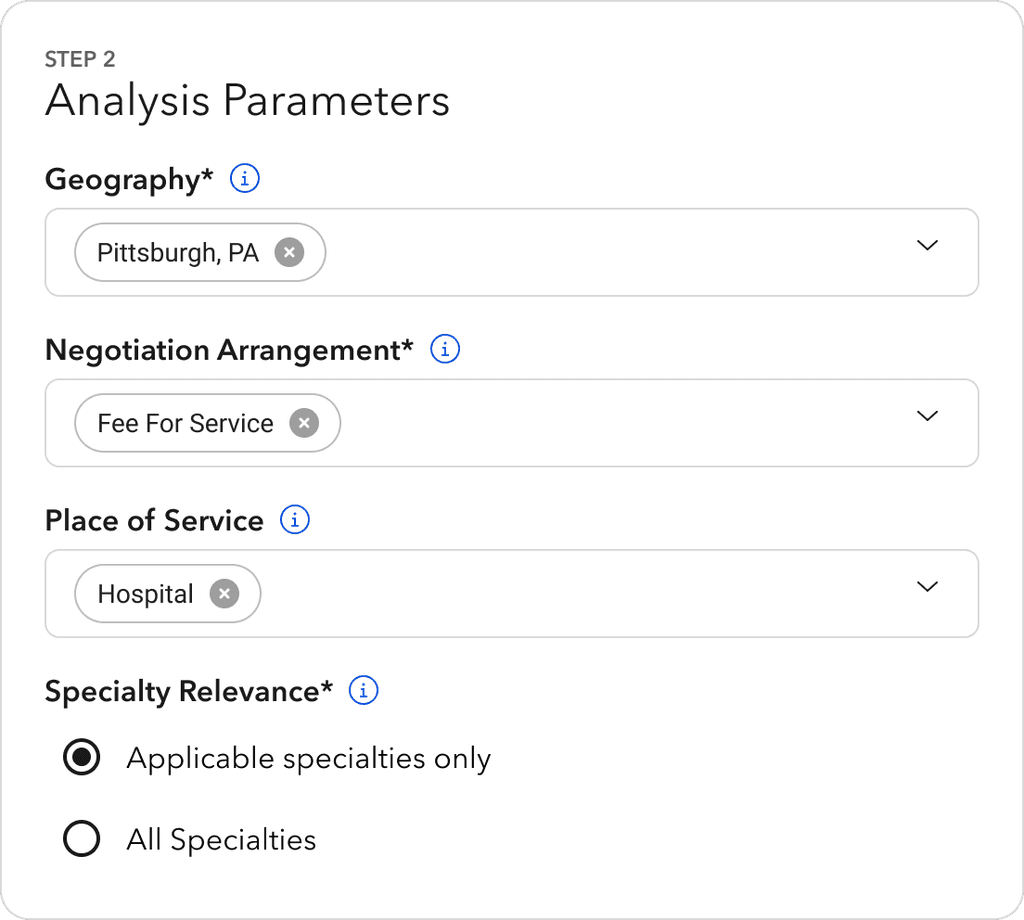

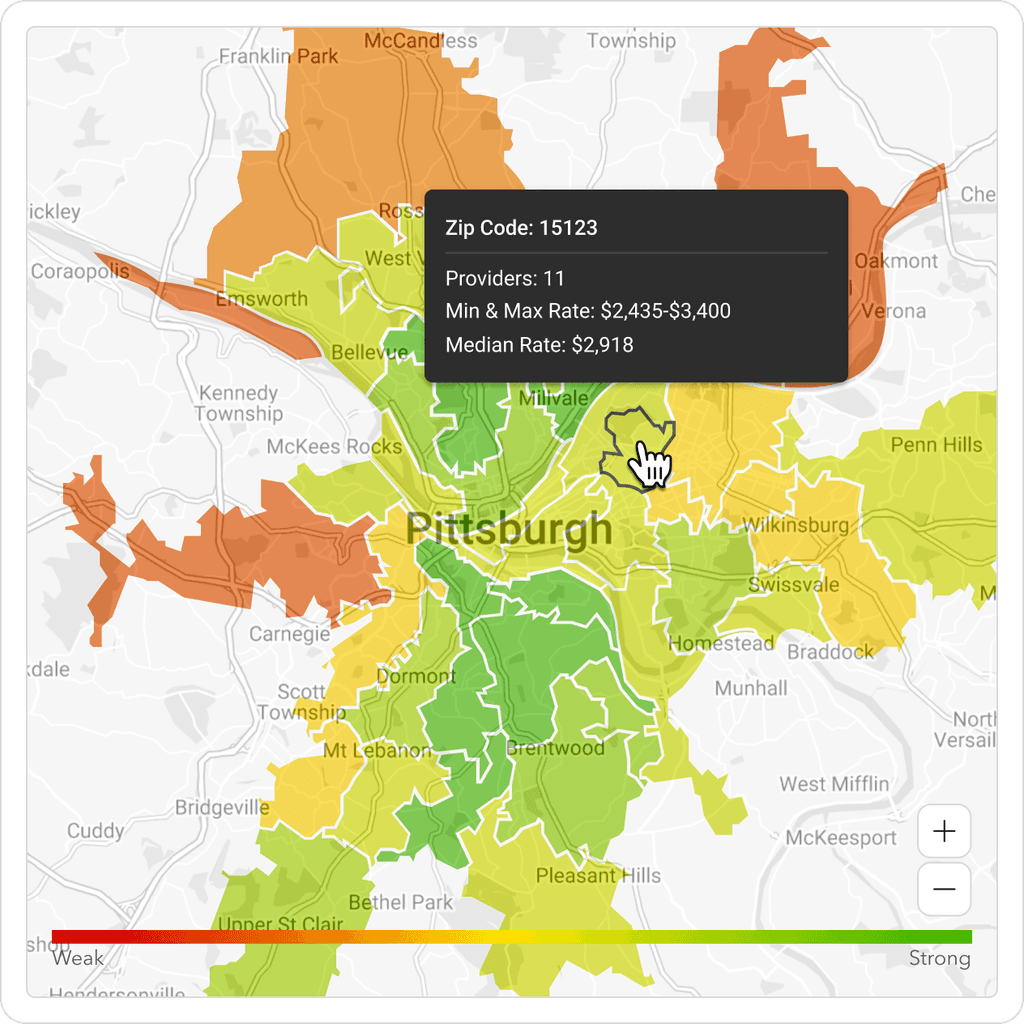

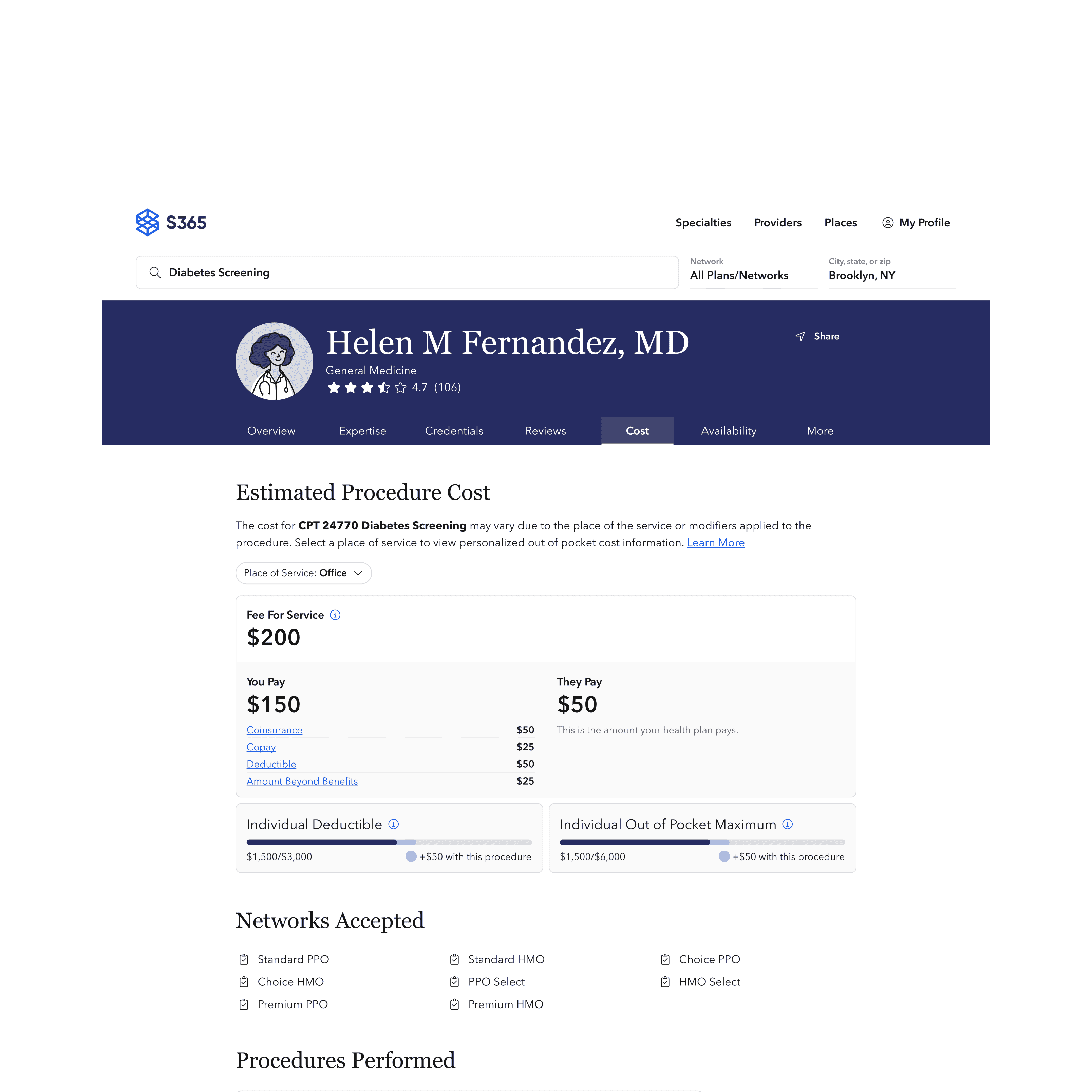
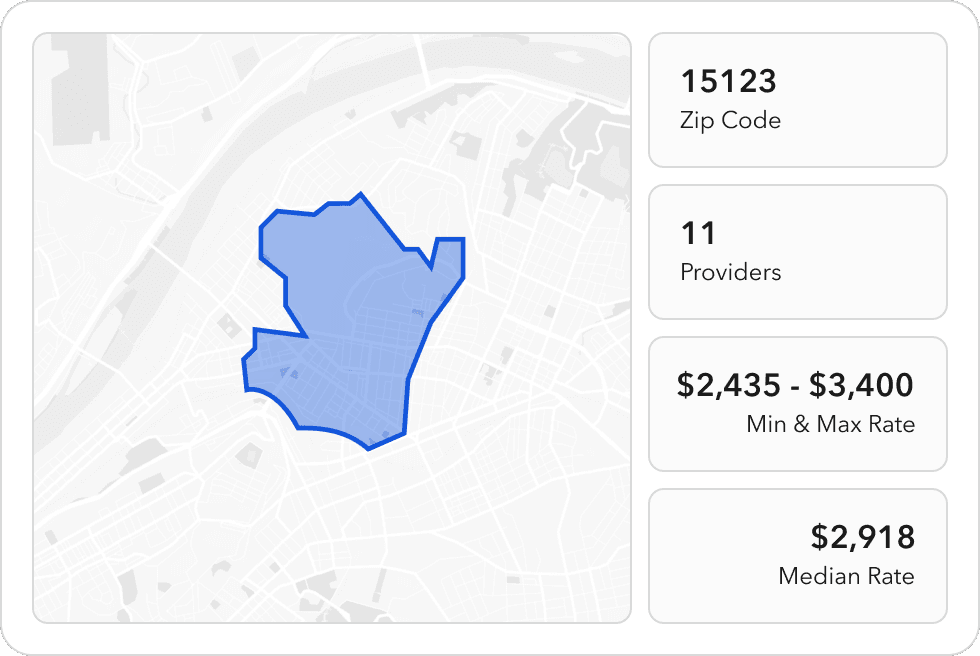
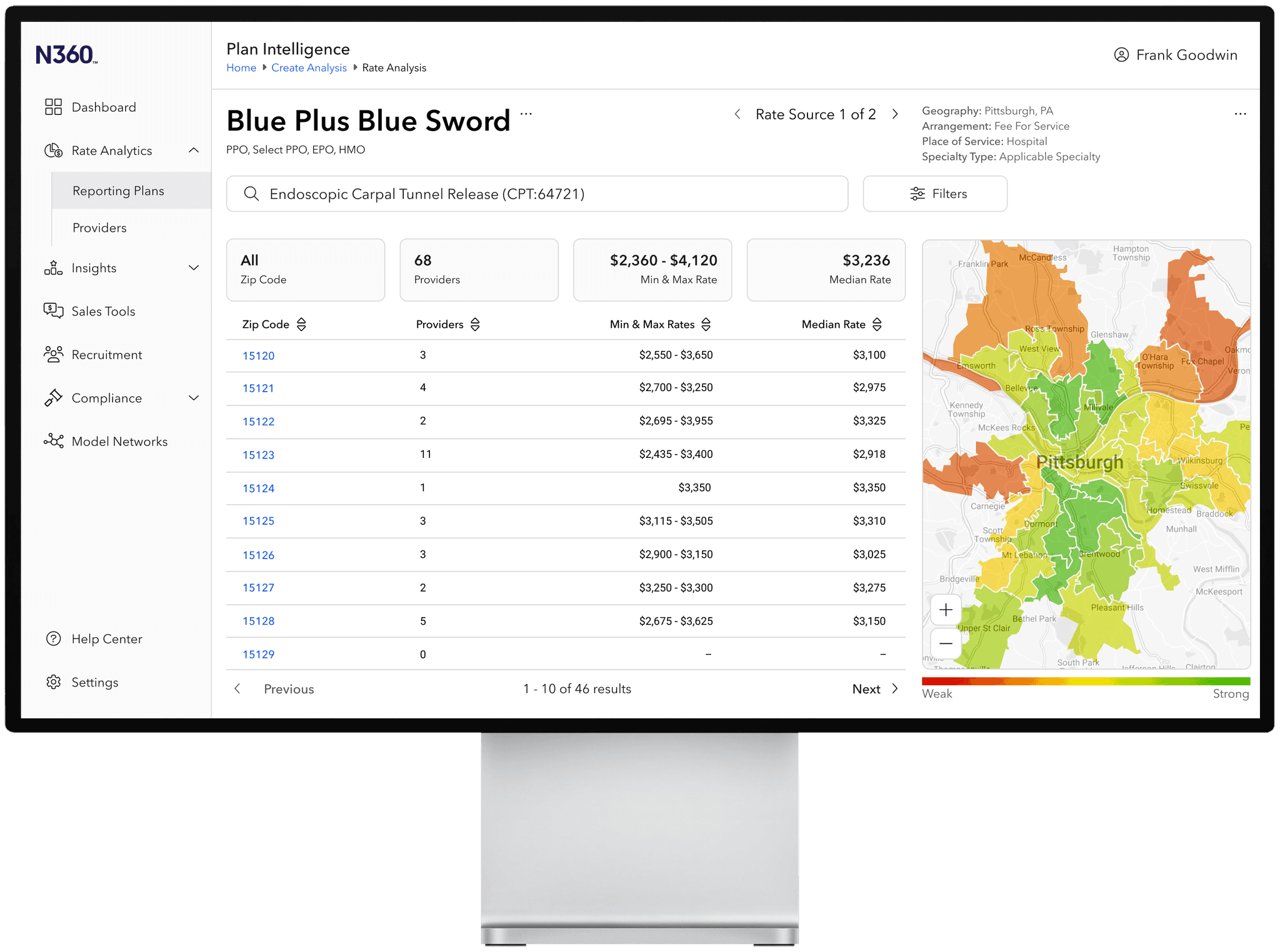
Geographic segmentation displays rich insights into the strength of a given provider network and portrays where competitor populations are being served.
Geographic segmentation displays rich insights into the strength of a given provider network and portrays where competitor populations are being served.
Geographic segmentation displays rich insights into the strength of a given provider network and portrays where competitor populations are being served.

/ Data Navigation
/ Data Navigation
/ Data Navigation
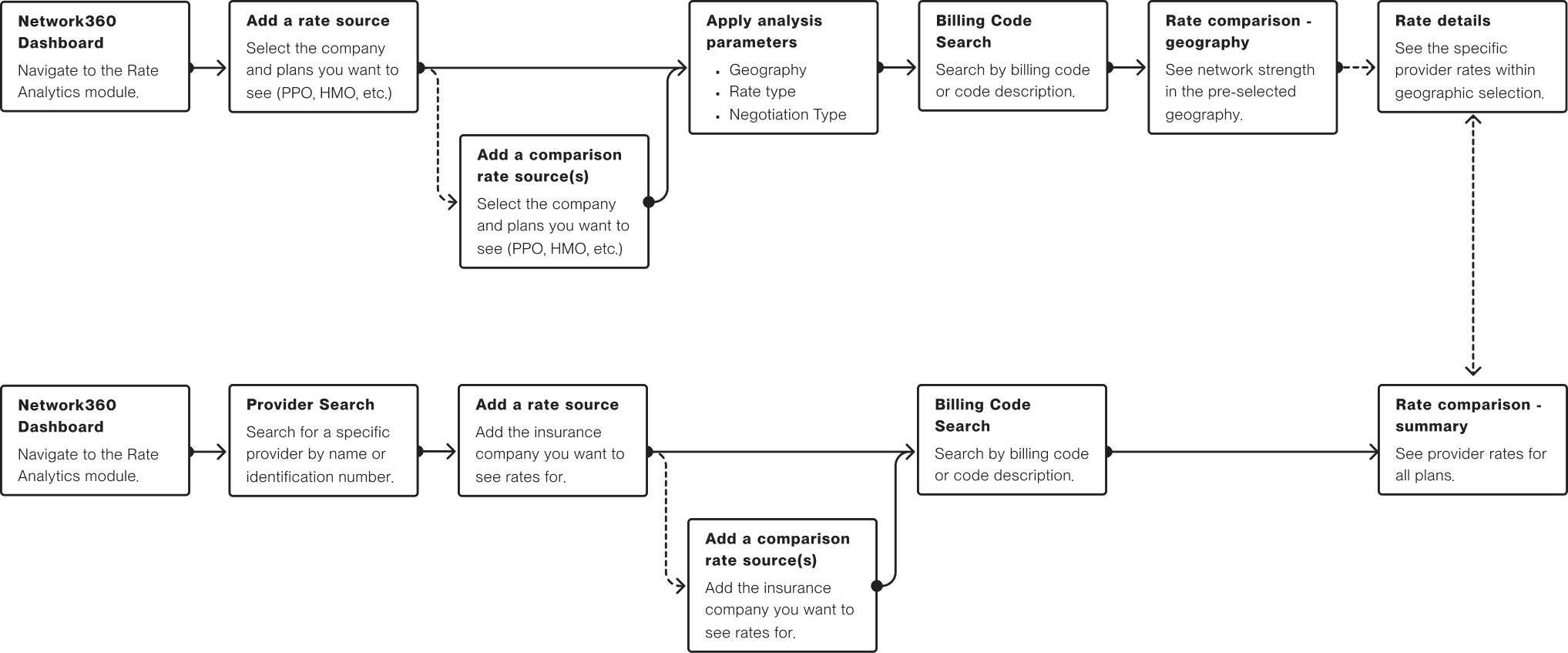
When looking for rate information, a network administrator may be looking for specific details or network patterns. Our user testing informed top-down (network first) and bottom-up (provider first) methods of navigating rate information.
When looking for rate information, a network administrator may be looking for specific details or network patterns. Our user testing informed top-down (network first) and bottom-up (provider first) methods of navigating rate information.
When looking for rate information, a network administrator may be looking for specific details or network patterns. Our user testing informed top-down (network first) and bottom-up (provider first) methods of navigating rate information.















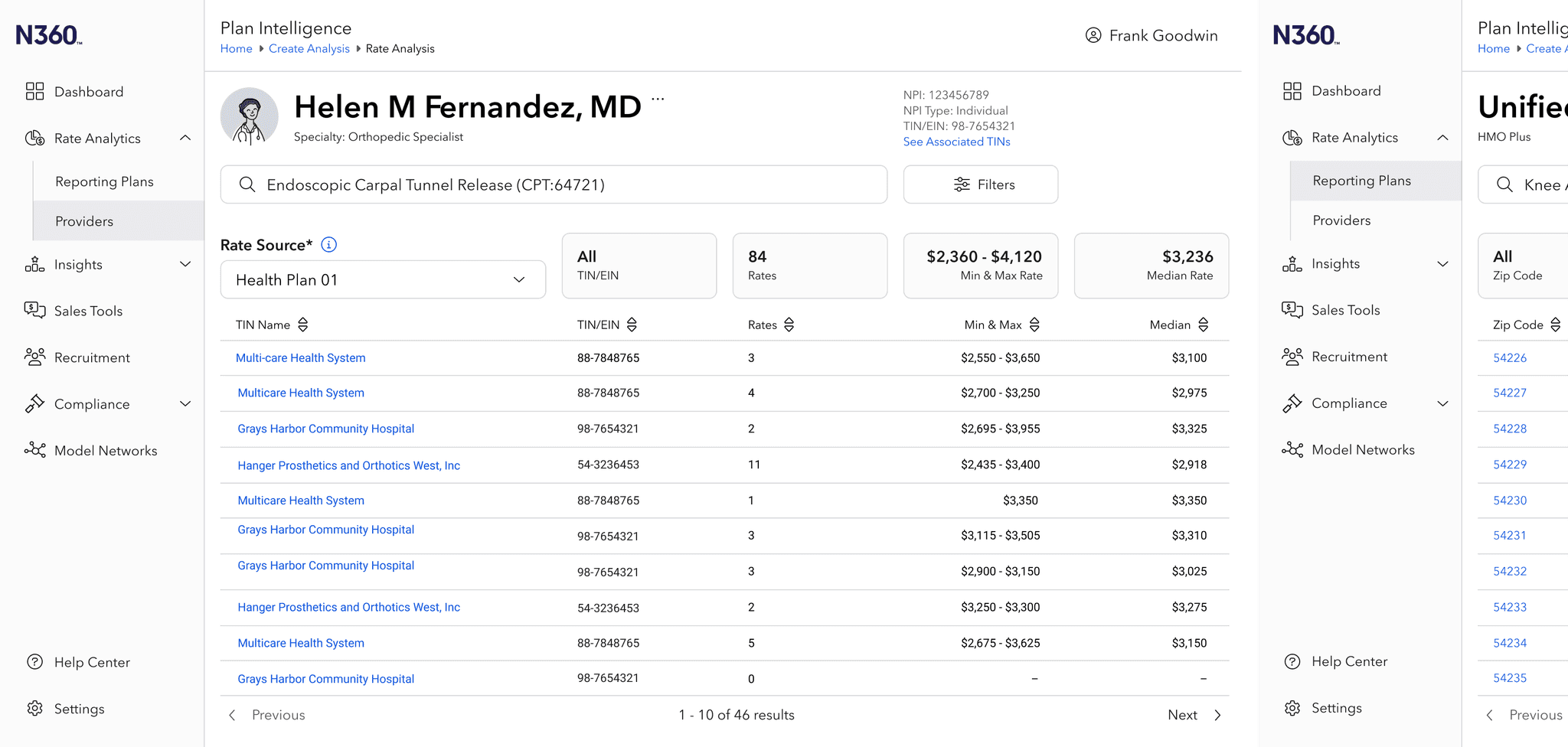
Named "Rate Analytics", the new module pulls from our cross-product interface design system to deliver a data analysis tool with rich data visualization and enhanced segmentation.
Named "Rate Analytics", the new module pulls from our cross-product interface design system to deliver a data analysis tool with rich data visualization and enhanced segmentation.
Named "Rate Analytics", the new module pulls from our cross-product interface design system to deliver a data analysis tool with rich data visualization and enhanced segmentation.


/ Outcome
/ Outcome
/ Outcome
This project initiated a formalization of product and design practices for this product that historically lacked investment. This included an interface migration to the organization design system, product analytics, and continuous product improvement, ultimately leading to improved client satisfaction and retention.
This project initiated a formalization of product and design practices for this product that historically lacked investment. This included an interface migration to the organization design system, product analytics, and continuous product improvement, ultimately leading to improved client satisfaction and retention.
This project initiated a formalization of product and design practices for this product that historically lacked investment. This included an interface migration to the organization design system, product analytics, and continuous product improvement, ultimately leading to improved client satisfaction and retention.
/ Reflection
/ Reflection
/ Reflection
Medical rate data is unstandardized, infrequently updated, and often inaccurate, which deteriorates the effectiveness of this tool. Until the Transparency in Coverage law is enforced, insurers will continue to delay providing satisfactory data.
We're actively exploring ways to grade the data quality in an attempt to encourage better data hygiene.
Medical rate data is unstandardized, infrequently updated, and often inaccurate, which deteriorates the effectiveness of this tool. Until the Transparency in Coverage law is enforced, insurers will continue to delay providing satisfactory data.
We're actively exploring ways to grade the data quality in an attempt to encourage better data hygiene.
Medical rate data is unstandardized, infrequently updated, and often inaccurate, which deteriorates the effectiveness of this tool. Until the Transparency in Coverage law is enforced, insurers will continue to delay providing satisfactory data.
We're actively exploring ways to grade the data quality in an attempt to encourage better data hygiene.